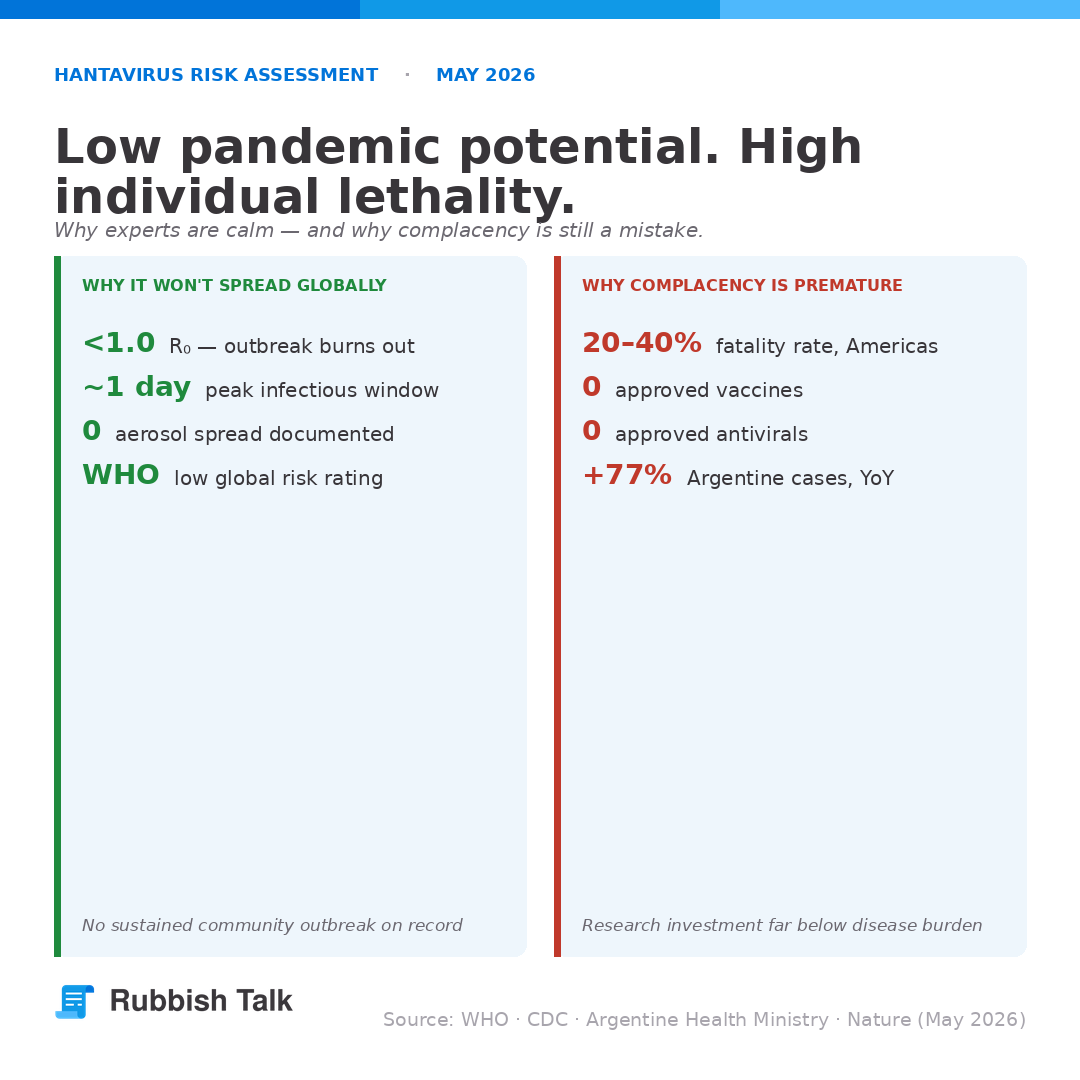
Summary
Three deaths linked to a Dutch cruise ship have put hantavirus on the front pages for the first time in decades. The outbreak, traced to the Andes strain circulating in Argentina, is serious but the global risk remains low. What receives far less attention: Argentine cases have nearly doubled year-on-year, the disease still has no approved treatment or vaccine after more than 30 years of surveillance, and the climate and land-use patterns driving the surge are getting worse, not better.
The Ship, the Strain, and What Actually Happened
On 1 April 2026, the Dutch expedition vessel MV Hondius departed Ushuaia, Argentina, at the southern tip of Patagonia, bound for the Antarctic and sub-Antarctic. Within ten days, a passenger was dead. By early May, two more passengers had died — one on board, one in a Johannesburg hospital after being airlifted off the vessel — and the World Health Organization had logged eight total cases, five confirmed as Andes hantavirus. WHO issued its first Disease Outbreak Notice on 2 May 2026.
The index case was a Dutch citizen who had spent the four months preceding embarkation on a road trip across Argentina, Chile, and Uruguay. Argentine health authorities subsequently traced his movements, mapping potential exposure sites across a region where hantavirus incidence has been climbing steadily. By the time he boarded the ship, he was almost certainly already infected. The narrow window for Andes virus transmission — peak infectiousness lasts approximately one day, coinciding with the onset of fever — meant that close contacts on board were at risk before anyone knew there was a problem.
The CDC classified its response at Level 3, its lowest emergency activation tier. Five US states were placed on monitoring for returning passengers. Multiple countries followed returning travellers. No secondary spread beyond the ship has so far been confirmed.
The Mainstream Narrative: Calm, But Incomplete
The dominant media framing since early May has been reassuring — and on the narrow question of pandemic risk, the reassurance is warranted. WHO Director of Epidemic and Pandemic Management Maria Van Kerkhove was unambiguous:
“This is not the start of a COVID pandemic.” — Maria Van Kerkhove, WHO Director of Epidemic and Pandemic Management, May 2026
Amesh Adalja, senior scholar at the Johns Hopkins Center for Health Security, reinforced the point with the relevant scientific reasoning:
“Pandemic potential is mostly about transmission architecture, not lethality. The biology that drives pandemics is how a pathogen moves between people — not how sick it makes them.” — Dr. Amesh Adalja, Johns Hopkins Center for Health Security, May 2026
These assessments are correct. The Andes virus, while the only hantavirus known to spread person-to-person, does so inefficiently. Those infected typically transmit to fewer than one additional person on average — an effective reproduction number below 1.0, which is the mathematical boundary between an outbreak that expands and one that burns out. Transmission requires close, sustained contact: the kind seen in households and healthcare settings, not casual proximity.
What the mainstream coverage has handled less well is the context behind the headline cases: why Argentina is seeing a significant and sustained increase, what resources exist to treat or prevent the disease, and what the data looks like when you zoom out beyond the cruise ship.
What the Data Actually Shows
Hantavirus is not a new pathogen. It has been tracked in the United States since 1993, when an outbreak in the Four Corners region — where Arizona, Colorado, New Mexico, and Utah meet — killed more than a dozen people and triggered the creation of a national surveillance system. Between 1993 and 2023, the CDC recorded 890 confirmed US cases. Of those, 309 people died — a case fatality rate of approximately 34%.
The global picture differs sharply by region and by strain. In Asia and Europe, where hantavirus typically causes haemorrhagic fever with renal syndrome (HFRS) rather than the cardiopulmonary syndrome (HCPS) seen in the Americas, fatality rates run below 15% and sometimes below 1%. Globally, an estimated 60,000 to 100,000 people are infected each year, with China accounting for roughly half of all cases. In the Americas, reported cases are far lower — 229 across the continent in 2025 — but the fatality profile is dramatically worse. The Andes and Sin Nombre strains carry case fatality rates of 20% to 40%.
Argentina’s current season, which began in June 2025, has been the worst in recent memory. The country recorded 101 confirmed cases through early May 2026 — nearly double the 57 cases during the same window the previous year. At least 32 people have died, a fatality rate of 31%. Significantly, the geographic footprint has shifted: hantavirus had long been associated almost exclusively with Patagonia, but this season the province of Buenos Aires recorded the highest case count of any region in the country. That is not a minor epidemiological note — it represents the disease moving into more densely populated territory.
Thirty Years of Surveillance, No Treatment
The most underreported fact about hantavirus is not its fatality rate. It is that after more than three decades of tracking the disease in the United States alone, there is still no approved antiviral treatment and no licensed vaccine anywhere in the world for the strains that cause the most deaths.
Management remains entirely supportive: oxygen, fluid balance, mechanical ventilation in severe cases. Ribavirin, an antiviral used against other haemorrhagic fevers, has shown no meaningful benefit in controlled trials for HCPS. The clinical picture moves fast — patients can deteriorate from mild flu-like symptoms to respiratory failure within 24 to 48 hours — and there is nothing disease-specific to give them.
“There is no vaccine for deadly hantavirus.” — Nature, May 2026
Vaccine research is active but early-stage. Moderna has conducted research on hantavirus in collaboration with the US Army Medical Research Institute of Infectious Diseases. A group at the University of Bath announced a new development programme in May 2026 directly in response to the MV Hondius outbreak. ORF Biologics, a smaller research company in Iowa, is targeting a diagnostic test within a year and a treatment within one to two years. None of these are on the immediate horizon for clinical use.
This is not the result of a uniquely difficult biology. It reflects, at least in part, where global research investment has historically flowed. Diseases that kill thousands in the Americas and tens of thousands globally — but mostly in rural and lower-income populations — have rarely commanded the same pharmaceutical interest as diseases with larger addressable markets.
Climate, Land Use, and the Expanding Risk Map
Experts attribute the surge in Argentine cases to two intersecting factors: climate change and habitat disruption. Both affect the rodent populations — primarily the long-tailed pygmy rice rat — that serve as the primary reservoir for the Andes virus.
Warmer and wetter seasons in parts of South America have driven increases in seed and food abundance that support rodent population booms. Simultaneously, agricultural expansion and ecotourism infrastructure have pushed humans into closer contact with rodent habitats. The index case in the MV Hondius outbreak spent four months travelling through precisely this territory before boarding his ship.
The broader pattern is not unique to South America. Climate change is reshaping the geographic range of hantavirus rodent hosts across multiple continents. In Europe, Puumala virus — which causes a milder form of the disease — has seen expanded distribution as bank vole populations shift northward. The World Health Organization has acknowledged that stronger surveillance systems, faster laboratory coordination, and more robust rodent-control measures are increasingly necessary as ecotourism and environmental disruption accelerate animal-to-human spillover events.
What Is Being Missed
Two items have received almost no coverage in the current outbreak cycle. The first is the geopolitical dimension of the US public health response. The US withdrawal from the World Health Organization — effective January 2025 — has complicated coordinated international tracking of the MV Hondius cases. The US is the country with the most developed hantavirus surveillance infrastructure in the Americas, and its departure from WHO information-sharing networks creates gaps precisely in the scenarios — a multinational outbreak linked to international travel — where that infrastructure matters most.
The second is what this outbreak reveals about global preparedness for zoonotic diseases with high case fatality rates and no treatment options. COVID-19 drove massive investment in mRNA vaccine platforms and pandemic surveillance systems, but that investment was reactive. Hantavirus has been killing people in the Americas at a 20–40% fatality rate for at least three decades, and the pharmacological toolkit available to treating physicians is unchanged from 1993.
What Comes Next
In the near term, the MV Hondius outbreak appears likely to remain contained. The Andes virus’s transmission biology — the short infectious window, the requirement for prolonged close contact — makes large-scale secondary spread unlikely. WHO has maintained its low global risk assessment, and no cases beyond the original cluster have been confirmed as of 9 May 2026.
The medium-term picture is harder to dismiss. Argentina’s doubling of cases over a single season, the geographic spread toward Buenos Aires, and the complete absence of therapeutic options all point to a disease that warrants significantly more research attention than it currently receives. The University of Bath and Moderna programmes are steps in the right direction, but they follow decades of relative neglect.
The variables to watch: whether any of the passengers who disembarked the MV Hondius before the outbreak was identified develop symptoms in the coming weeks; whether Argentina’s case count continues its upward trajectory through the remainder of the southern hemisphere autumn; and whether the current outbreak accelerates vaccine development timelines in any meaningful way, or dissipates with the next news cycle.
Hantavirus is not the next pandemic. But the conditions enabling its spread — climate disruption, habitat encroachment, ecotourism growth — are structural rather than episodic. The disease will keep arriving in headlines. The question is whether that prompts a sustained research response, or another round of temporary concern.
Sources:
- WHO Disease Outbreak Notice DON599
- WHO Disease Outbreak Notice DON600
- CDC Hantavirus Cases Data
- CDC MV Hondius Update
- Nature — No vaccine for hantavirus
- CNN — Argentina cases double, climate change
- Bloomberg — Moderna hantavirus research
- NPR — Hantavirus likely not the next COVID
- NBC News — US WHO departure
- Harvard T.H. Chan — Pandemic risk
- Wikipedia — MV Hondius outbreak
- Foto: Stefan Brending / Lizenz: Creative Commons CC-BY-SA-3.0 de